Living with Cystic Fibrosis (CF) has been a very difficult challenge for me. I, and the 30,000 other people in the U.S. that have it, face challenges of many calibers including physical, social, and economic issues. It affects my physical being, my platonic and romantic relationships, and my financial well-being.
CF is the most common, fatal genetic disease in the United States. It has the biggest impact on the lungs, but it also affects the pancreas and liver. The pancreas and liver issues aren’t the main reason for concern. Sure, the intermittent diarrhea, abdominal pain and constipation that we frequently deal with may seem like a big deal to most healthy adults. But the reality is, those gastrointestinal issues pale in comparison to the toll that the pulmonary issues take on us. Chest tightness, congestion, chronic coughing, and overall exhaustion are something we can experience every day.
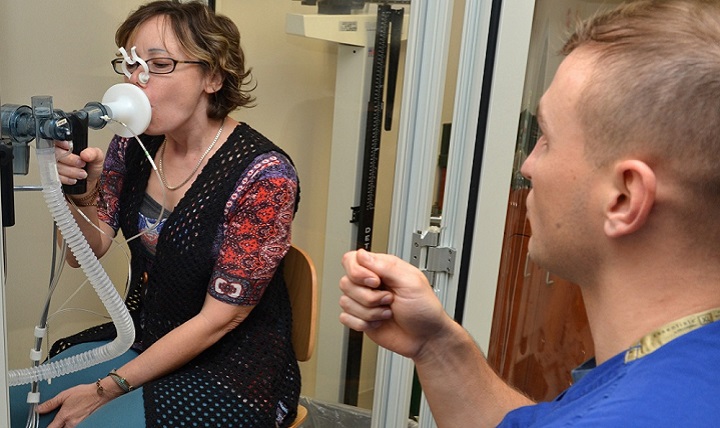
Some days are better than others. But generally speaking, every year is worse than the last. CF patients take quarterly pulmonary function tests and watch as our lungs go from 100% relative function as a child, to 10% function later in life, at which point we are at the brink of death. It becomes impossible to take a deep breath (you will cough if you try,) and it feels like you’re breathing through a straw. At this point you are bedridden until you are lucky enough to get a lung transplant, or you slowly wither away in pain.
People want to sympathize, so they ask questions. Even though I know that they’re only asking the questions because they care, it still hurts. I get asked so many times if I’m okay. Usually I brush it off and say “yea I’m fine.” Sometimes I’ll give a more genuine response like “I could be better.” But there are so many times where I just want to scream out the truth. No I’m not fine. I wake up every day feeling just a little bit worse than the last. I’m working towards a bachelor’s degree but it might be futile in the end and not just because of the shot clock that’s quickly counting down on my life. If I can’t find a job with comprehensive health benefits to cover the tens of thousands of dollars that my medications cost each month, then all these years working hard to maintain good grades in high school and college have been futile. I may as well live off of the government’s medicare like I do now –something which I can only do if I’m not employed.
It’s easy to take in all this information and fall deep into a spiral of negative thoughts and feelings. There have been times where I wish I was already taking my dying breaths, because then I would be put on a lung transplant list. I would either die waiting for a new pair of lungs, or I would get a new pair of lungs and hope that I’m part of the 50% of lung transplant recipients that live over 10 years. It is especially hard to deal with these internal conflicts when I remember my uncle Juan, who died to CF before I was even born.
However, you have to keep your head up high. The beauty of life isn’t about the destination you reach at the end. It’s about the experiences and friends you make along the way. So it’s important for people with CF to build a good network of support from friends and family. Because when things are rough and you’re feeling down, you know that they’ll have your back. But this also means people with CF need to reach out, and that’s a lesson I’m trying to learn.